Provider Risk Management Is Hard to Do
-
December 01, 2021
DownloadsDownload Article
-
Enterprise risk management in health care “comprises the clinical and administrative systems, processes, and reports employed to detect, monitor, assess, mitigate, and prevent risks1.” Historically, risk management in health care has focused on patient safety and the avoidance of medical errors. It has now expanded to consider the entire enterprise, inclusive of strategic, operational, financial, human capital, legal/regulatory and technological risk2.
The advent of value-based care based on the “Triple AIM” framework developed by the Institute for Healthcare Improvement — improving the individual experience of care, improving the health of populations, and reducing the per capita costs of care — has pressured providers to shift their focus from volume to value3. And, as providers shift to value-based activities, their reimbursement model is also more in alignment with that of payers. Like payers, providers now benefit from a fundamental understanding of and ability to manage risk.
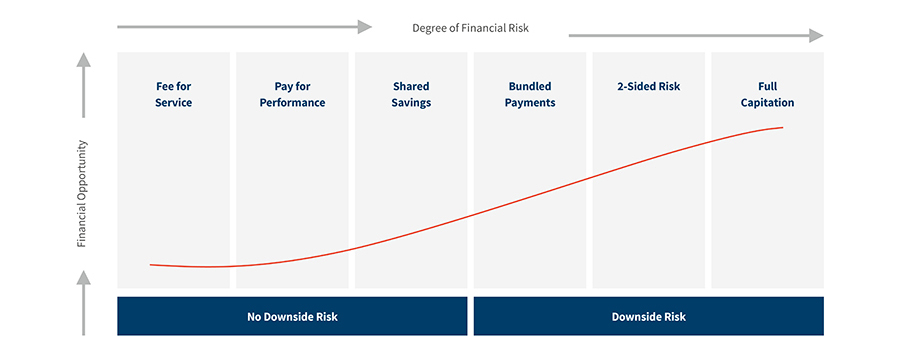
Taking risk offers strategic, financial and technological opportunities for provider groups. As providers take on more accountability for patient care in exchange for greater reimbursement, they should understand the degree of risk-sharing associated with alternative business models. For example, the transition into risk-sharing can be gradual, beginning with pay-for-performance or one-sided shared savings opportunities and, with increasing experience, can extend to a full risk commitment consisting of global capitation.
Continuum of financial risk to providers
Source: FTI Consulting
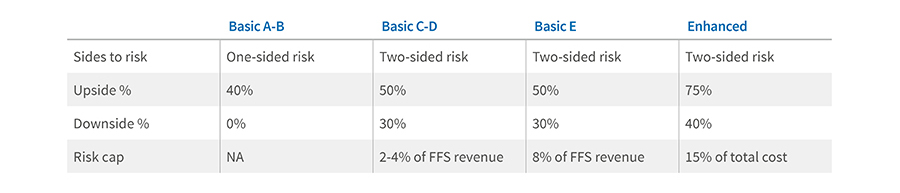
In 2021, approximately 11.9 million Medicare beneficiaries were enrolled in 518 Accountable Care Organizations; 10.7 million (90 percent) in Medicare Shared Savings Program (MSSP) and 1.2 million (10 percent) in Next Generation ACOs4,5. The MSSP requires ACOs to meet quality and performance benchmarks, then offers shared savings when the ACOs achieve their goals. A minimum of 5,000 members is required by the Centers for Medicare & Medicaid Services (CMS) for an ACO to participate in a shared savings program. As of January 1, 2021, the majority of MSSP participants, 59 percent, were enrolled with one-sided, upside-only risk, and the remaining 41 percent were enrolled with two-sided, upside/downside risk6. Next Generation ACOs allow participants to assume higher levels of risk and potentially higher rewards. The program is ending after this year7.
Medicare Shared Savings Plans (MSSP)
Shared Savings Program Participation Options for Performance Year 2022
https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/Downloads/ssp-aco-participation-options.pdf
In 2021, 26.4 million people, or 42% of the Medicare population, were enrolled in Medicare Advantage (MA) plans8. The Congressional Budget Office projects a 46% share in 2025 and 51% by 20309. MA plans receive a fixed revenue per member per month (PMPM) based on the demographics of the plan’s member population, overall level of health (e.g., risk-adjusted factor score) and quality bonuses (e.g., STARS)10. Offsetting the revenues are health-related costs (i.e., Medical Loss Ratio) and SG&A.
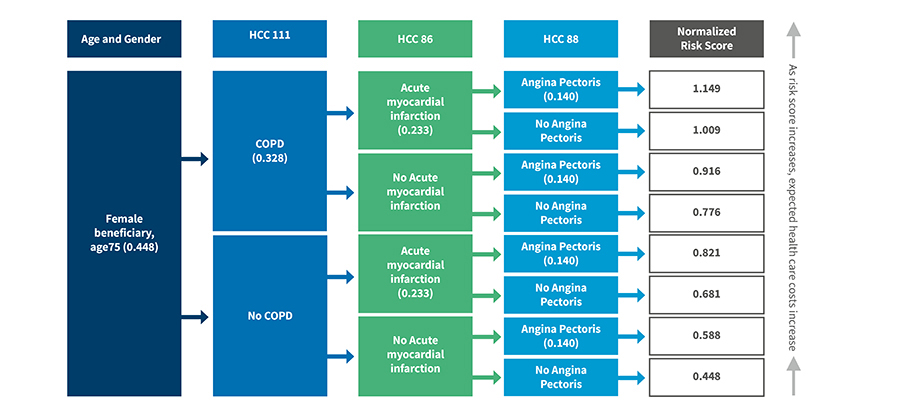
The calculation of the Medicare Advantage risk-adjustment factor begins by grouping ICD-10 codes into DxGroups that represent a medical condition11. The DxGroups are then combined into Condition Categories “that are similar clinically and in terms of costs12.” Hierarchies are imposed such that a person is coded with the “most severe manifestation of disease13.”A Hierarchical Condition Category is used to risk-adjust Medicare Advantage base rates, the lower of a plan’s bid or benchmark (the average fee-for-service Medicare spending in each county adjusted for demographics and geography).
Medicare Advantage Risk Adjustment Example
Understanding Medicare Advantage Payment and Policy Recommendations. Better Medicare Alliance; September 2018.
https://bettermedicarealliance.org/wp-content/uploads/2020/03/BMA_WhitePaper_MA_Bidding_and_Payment_2018_09_19-1.pdf
The attractiveness of capitation increased during the pandemic when ambulatory volume declined. Key success factors include: (1) minimal size of the risk pool for risk dispersion; (2) the primacy of proactive (preventive) intervention, acute and post-acute care by primary care physicians; (3) risk stratification with an increased focus on the 18% of patients accounting for 54% of costs; (4) availability of tools (analytics) and resources to manage care; and (5) health plan contractual arrangements with cost-effective specialists on a discounted fee-for-service or sub-capitation basis.
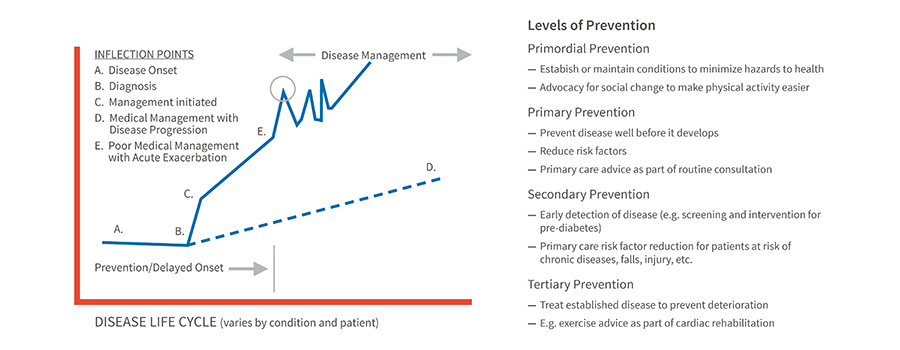
Managing the total cost of care is essential. The chronic disease life cycle is typically progressive, subject to acute, intermittent events and best managed by primary care physicians; acute episodes of care to 90 days post-discharge accounts for 50% of Medicare spending14. The Institute of Medicine has attributed 73 percent of overall Medicare geographical spending variances to variations in post-acute care utilization15. Social determinants of health – “the conditions in the environments where people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks” – also affect engagement and outcomes16. Only 1.59% of Medicare FFS beneficiaries had a Z-code (social determinant) claim17.
Shifting provider focus to chronic disease management from acute intervention to prevention, monitoring, and proactive intervention
Source: FTI Consulting
Risk pool viability requires sufficient size comprised of a broad section or risks. The goal of risk pooling is to share the costs of a sick population across a broader (healthier) population. Insurance companies and health plans strive to grow their membership to spread this risk and diversify across product lines to offset financial fluctuations in one group versus the other. Today, risk-bearing provider organizations are no different, with the successful provider organizations managing a large number of at-risk members (minimum of 5,000 members) and risk relationships across different populations – commercial, Medicare Advantage, Managed Medicaid and self-insured.
Bottom Line:
With the continued transition to value-based care, providers have an increased opportunity to participate in at-risk relationships with payers, both public and private. Success in these programs requires providers to develop skills and competencies outside their traditional clinical expertise. The transition isn’t always easy, but the rewards are promising.
Footnotes:
1: What Is Risk Management in Healthcare? NEJM Catalyst; April 25, 2018 https://catalyst.nejm.org/doi/full/10.1056/CAT.18.0197
2: ASHRM Enterprise Risk Management: Framework and Domains. https://www.ashrm.org/system/files?file=media/file/2019/06/ERM-Tool_final.pdf
3: Institute for Healthcare Improvement http://www.ihi.org/Engage/Initiatives/TripleAim/Pages/default.aspx
4: Centers for Medicare & Medicaid Services — Shared Savings Program Fast Facts—As of January 1, 2021. https://www.cms.gov/files/document/2021-shared-savings-program-fast-facts.pdf
5: Susan Morse. Updated with list: Majority of Next Generation ACOs earned shared savings. Healthcare Finance; January 15, 2021 https://www.healthcarefinancenews.com/news/majority-next-generation-acos-earned-shared-savings
6: Centers for Medicare & Medicaid Services — Shared Savings Program Fast Facts—As of January 1, 2021. https://www.cms.gov/files/document/2021-shared-savings-program-fast-facts.pdf
7: Robert King. Biden admin to end Next Gen ACO model after this year. FIERCE Healthcare; May 21, 2021 https://www.fiercehealthcare.com/hospitals/biden-admin-ends-next-gen-aco-model-after-year
8: Meredith Freed, Jeannie Fuglesten Biniek, Anthony Damico, and Tricia Neuman. Medicare Advantage in 2021: Enrollment Update and Key Trends. KFF; June 21, 2021 https://www.kff.org/medicare/issue-brief/medicare-advantage-in-2021-enrollment-update-and-key-trends/
9: Ibid.
10: Understanding Medicare Advantage Payment & Policy Recommendations. Better Medicare Alliance; September 2018, p. 9. https://bettermedicarealliance.org/wp-content/uploads/2020/03/BMA_WhitePaper_MA_Bidding_and_Payment_2018_09_19-1.pdf
11: Ibid.
12: Ibid.
13: Ibid.
14: 5 Keys to Managing Total Cost of Care for Acute Episodes. Sound Physicians Webinar https://soundphysicians.com/webinar/5-keys-to-managing-total-cost-of-care-for-acute-episodes/
15: Variation in Health Care Spending: Target Decision Making, Not Geography. Institute of Medicine; 2013 http://nap.edu/18393
16: Utilization of Z Codes for Social Determinants of Health among Medicare Fee-for-Service Beneficiaries, 2019. CMS Data Highlight #24; September 2021 https://www.cms.gov/files/document/z-codes-data-highlight.pdf
17: Ibid.
Related Insights
Related Information
Published
December 01, 2021
 Key Contacts
Key Contacts
Senior Managing Director