Blocking and Tackling the Revenue Cycle
-
February 24, 2022
DownloadsDownload Article
-
To no one’s surprise, the revenue cycle plays an integral role in, and has a significant impact on, cash flow. The revenue cycle includes front-end activities such as scheduling, authorization management, insurance verification and pre-registration/registration; mid-cycle activities such as charge capture and coding; and back-end activities such as: claims submission, claims follow-up, denials management, payment posting and customer service. This complicated maze of interworking and prioritization oftentimes results in inefficiencies and opportunities for improvement.
In this article, we focus on a back-to-basics approach for “back-end” accounts receivable management techniques that serve to increase cash flow, boost net revenue, reduce “days revenue in accounts receivable” and lessen denials.
These “Top 10” basic “blocking-and–tackling” techniques require an orchestration of duties throughout the revenue cycle, coupled with prioritization of collection efforts and enhanced denials management. Many of these “Top 10” activities are well-known by tenured revenue cycle professionals, but, given time constraints and the demands of everyday work, are often overlooked.
In addition to these techniques, we suggest a regular comparison of your Key Performance Indicators (KPIs) to industry benchmarks, which will serve as a roadmap to assure that your revenue cycle is trending in the right direction. These benchmark comparisons provide an early indicator to course-correct when needed and help drive future business decisions.
Our “Top 10” basics for back-end revenue management fall into the following main categories:
“Clean Claims” Submission and First Pass Yield:
These terms refer to the percentage of UB-04 claims and CMS 1500 forms that pass all internal edits in a provider’s claim “scrubber” and are accepted into a payer’s processing system without human intervention. Understanding a provider’s clean claim rate includes reviewing the frequency of edits by error code, by payer, that cause claims to fail in your bill scrubber. Best practices include building edits as far upstream in the revenue cycle as possible to improve an organization’s ability to produce clean claims. Coupled with the clean claims rate, an organization’s First Pass Yield percentage represents the percentage of claims being processed correctly upon first submission to a payer. A higher First Pass Yield indicates that strong claims edits and low denials rates are in place. As a rule, high-performing organizations achieve a benchmark of 95% or better for both Clean Claims Rate and First Pass Yield.
Quick, Timely and Efficient Billing of Claims:
An internal focus with both coding and documentation supports quick throughput of claims from service date to submission. Two common measures to review efficiency involve the throughput of Discharged Not Final Coded (DNFC) and Discharged Not Final Billed (DNFB) accounts. DNFC and DNFB are complementary measures, with DNFC focused on completion of coding and documentation requirements necessary before claims submission, and DNFB focused on claims/billing edits required before submission. The combined DNFC/DNFB benchmark for high-performing health systems is < 5 days. Once claims are generated, a provider should also track Final Bill Not Submitted (FBNS) in the claim scrubber to ensure that claim errors are worked in a timely fashion. As a best practice, organizations should resolve claim errors and transmit claims from the claim scrubber to insurance carriers daily.
Knowing Payer “Timely Filing” Rules:
Incorporating payer timely filing guidelines for initial claims submission, rebills, corrected claims and appeal filing windows into the RCM/work-driver is vital to assure that claims are submitted and followed up with payers timely and within their contracted parameters. Untimely write-offs are one of the key avoidable adjustments that providers should evaluate since the result causes a direct reduction to revenue. Additionally, best practices involve the use of timely filing logic within a provider’s work driver, coupled with workflow methodologies that prioritize accounts as they approach an untimely filing window and keep timely filing adjustments within focus and avoidable.
Account Prioritization and Follow-up Intervals:
Setting appropriate workflow priorities to balance available resources with accounts that require follow-up is necessary for an efficient and successful revenue cycle operation. To achieve balance, organizations should continually evaluate their staffing needs by performing a staffing analysis as volumes change; this will help determine the staffing complement needed to process claims efficiently. Additionally, if patient volumes exceed a provider’s ability to process or follow-up on claims, an effective outsourcing strategy should be employed to handle the volume of accounts not being addressed. In addition, the age, payer and balances of accounts should be considered when setting workflow prioritization. Typically, higher dollar balances and/or younger claims should be prioritized with quicker interval periods of 14–21 days between touches. Best practices achieve 80% or more of their billed A/R pays within the first 60 days of service date. Therefore, it is important to understand the average days to pay for each insurance company to avoid unnecessary touches and to also prioritize tickle timeframes for outstanding accounts receivable. Lastly, automating claim status inquiries for payer responses and integrating them into the practice management system can help reduce the number of touches and overall cost-to-collect.
Proactive Denials Management:
While every organization strives for a high First Pass Yield rate, it is likely that any organization will encounter denied claims. Understanding how to overturn and prevent future denials is integral to efficient revenue cycle management. Key steps in a denial management program include reviewing payer 835 files, the electronic transaction that provides claim payment information, to uncover denial trends, developing internal feedback loops to provide information to departmental stakeholders, providing training to team members to prevent reoccurrence, and reporting/measuring improvements. Forming a denials committee with active stakeholder involvement focused on denial prevention strategies is a best-in-class model. A good benchmark to strive for is a denial rate < 5% of gross revenue.
Payment Validation:
Providers should have the ability to comply with payer requirements and validate the accuracy of paid claims. Many providers use sophisticated software packages that model a payer’s expected benefits and compare those to the actual payment. Industry best practices include quick identification of payment variance amounts, analyzing refund requests for accuracy, and establishing a meeting cadence with a provider’s largest payers to address issues and contract compliance.
Human Capital (Workforce) Management:
In today’s environment, finding and keeping qualified staff is challenging. Having the basics of clear job descriptions, training programs, onboarding plans for remote workers, effective interview techniques and competitive salary/benefits is essential for every organization. Additionally, having the ability to manage a mostly work-from-home (WFH) workforce is critical to success today. Camera-on check-ins and group discussions are some of the most common ways to keep your WFH staff members engaged. Constant communication is vital to assuring that employees feel connected to their employer and team in a remote environment. Best practices involve the use of tools beyond Zoom, Teams, Hangouts, etc., but ones that can assist with structured performance feedback and employee recognition to keep communication top of mind.
Vendor Management:
Keeping the bar high for a provider’s outsourced vendors will help achieve overall goals for the revenue cycle. Too often, revenue cycle managers rely upon their outsource vendors in a “place and forget” mindset because of other competing priorities. Many providers think that they can do it themselves but eventually find out that many third-party accounts fall off the radar screen as they age with little to no follow-up. Effective outsourcing strategies can help bridge the gaps between reprioritizing your workforce to work the highest balance and younger accounts and employing an outsourcing strategy to place smaller-balance and older accounts with a vendor. Best-practice vendor management includes monthly dashboard reporting to track performance of outsourced inventory, routine touchpoints, invoice auditing and creation of Service Level Agreements before contract signing.
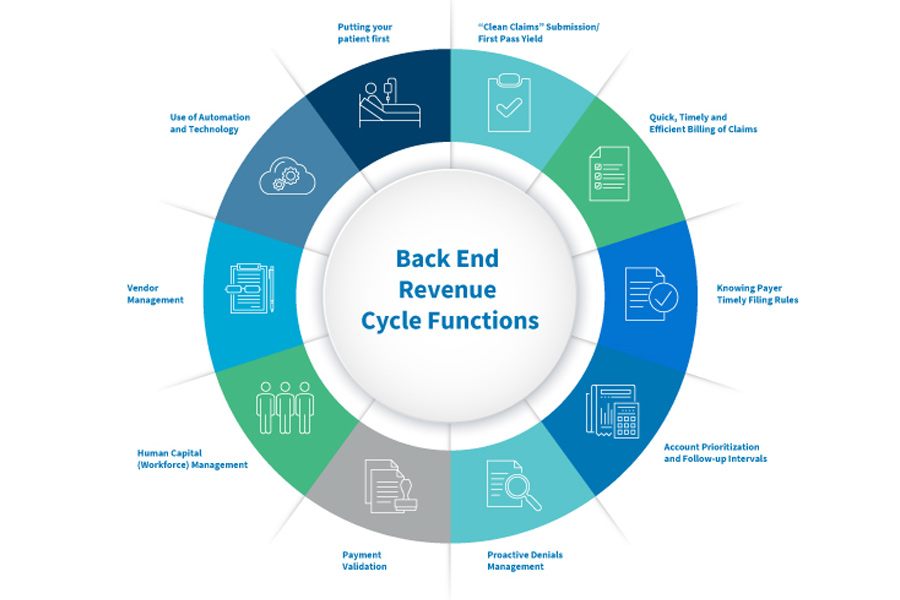
Use of Automation/Technology:
Vital to today’s revenue cycle is the use of Robotic Process Automation/Artificial Intelligence (RPA/AI) technology to streamline operational efficiencies. RPA/AI technology can be deployed to reduce the number of human touches associated with each account while also encouraging team members to only work accounts that require intervention, thereby making the job more challenging and engaging to revenue cycle staff members. Reducing the overall number of touches will also translate into a much lower overall cost-to-collect. Automation is increasingly common in today’s revenue cycle; most providers apply the technology to claims status, payment posting, credit balance remediation and a host of other manual functions that can be replaced with automation.
Putting Your Patient First:
Taking a patient-centric approach is a must for all providers. The patient's experience is not solely defined by the medical care they receive. Patients expect excellent service and communication at every touchpoint, which includes everything from ease of registration and scheduling, friendly and accurate customer service call responses, access to health information via a patient portal, to the development of patient-friendly statements that are understandable and encourage a variety of payment options.
Bottom Line
Getting back to the basics within the revenue cycle is often overlooked, but represents a vital component of any high-performing revenue cycle. Keeping the pillars of an effective accounts receivable strategy in the forefront includes efficient use of resources, balance in workflow, proactive denials management, account prioritization techniques and reducing redundancies in processes. Employing a strategy that involves a strong back-end workflow, which includes quality edits and preventive measures in patient access, health information and coding, will also assure that you are building a sustainable, healthy revenue cycle that submits clean claims to payers for prompt and accurate reimbursement.
Related Insights
Related Information
Published
February 24, 2022
 Key Contacts
Key Contacts
Senior Managing Director, Leader of Healthcare Business Transformation
Managing Director
Managing Director
Downloads
Most Popular Insights
- Beyond Cost Metrics: Recognizing the True Value of Nuclear Energy
- Finally, Pundits Are Talking About Rising Consumer Loan Delinquencies
- A New Era of Medicaid Reform
- Turning Vision and Strategy Into Action: The Role of Operating Model Design
- The Hidden Risk for Data Centers That No One is Talking About


