Change Management: Theories and Practice
Part 2 of 2: Change Management
-
January 28, 2022
DownloadsDownload Article
-
In a prior article, we discussed the imperative for change in patient care delivery driven by a rapidly aging population, physician shortages, hospital/health system direct employment models and the evolution of value-based care. While this opportunity has existed for quite some time, it has just recently gained criticality with the confluence of these factors.
In this article, we discuss negative perceptions among physicians as a barrier to change, change at the individual and institutional level, and the practical steps necessary to effect change, featuring lessons learned by FTI Consulting experts while serving in operational roles.
Negative Perceptions Among Physicians
A biennial survey from the Physicians Foundation in 2018 found somewhat negative or very negative perspectives on the current and future state of the medical profession1. Only 13.3% of those surveyed agreed, or strongly agreed, that hospital employment of physicians is likely to enhance quality of care and decrease costs2. The current state of relations between hospitals and physicians was described as somewhat/mostly negative and adversarial by 46.4%3. Most physicians surveyed (62.5%) believed they have little, or very little, ability to influence the healthcare system4. Only 18.0% agreed, or strongly agreed, that value-based compensation is likely to improve quality of care and reduce costs5. A list of the least satisfying factors about medical practice included EHR design/interoperability (39.2%), regulatory/insurance requirements (37.6%) and loss of clinical autonomy (37.0%)6.
In summary, physicians believe they have little influence; they are not supportive of value-based care; and they don’t believe hospital employment will improve care delivery. Physicians will be critical to the emergence of a value-based system; change is required.
Improving Perspective on Medical Profession, Though Plurality Still Negative
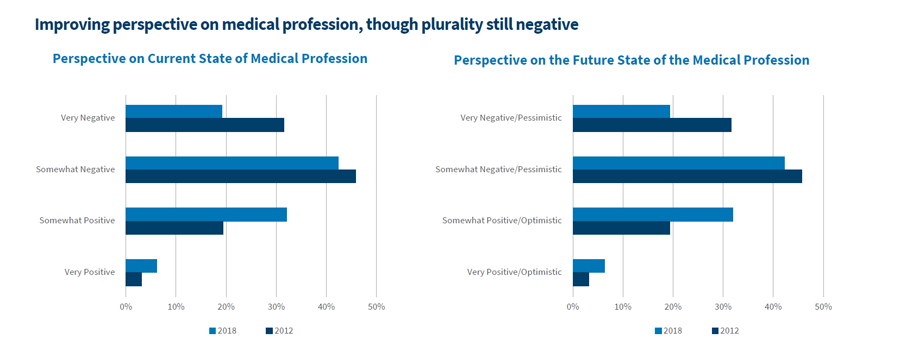
Physicians Foundation Survey, 2018. https://physiciansfoundation.org/wp-content/uploads/2018/09/physicians-survey-results-final-2018.pdf
Change at the Individual Level
There are many different models of behavioral change, including: Prochaska’s transtheoretical model (i.e., six stages of change: precontemplation, contemplation, planning, action, maintenance and termination); the theory of planned behavior (i.e., behavioral achievement depends on both motivation and ability); Bandura’s social cognitive theory (i.e., human behavior is learned through cognitive, behavioral and environmental factors); and social network theory (which views social relationships in terms of a network of nodes (individuals) and ties (relationships))7,8,9,10. Each of these models has the individual at the center, processing information, which ultimately results in change (or relapse).
Considerable variation exists regarding the time required for behavioral change. A study from the European Journal of Social Psychology found a range of 18-254 days to form a new habit11.
Change at the Institutional Level
Multiple frameworks for change exist at the institutional level, including the ADKAR (awareness, desire, knowledge, ability, reinforcement) model, the McKinsey 7-S model (shared values, strategy, structure, systems, style, staff), the Bridges Transition model (ending, losing, and letting go; the neutral zone, the new beginning) and the Kotter 8-step process (creating a climate for change, engaging and enabling the organization and implementing & sustaining for change)12,13,14,15.
We will be using the Kotter process to illustrate the challenges of institutional change in an evolving ecosystem that varies by local market. Creating the climate for change has three components: creating urgency, forming a powerful coalition and creating a vision for change. Engaging and enabling the organization involves communicating the vision, empowering action and, importantly, creating quick wins. Quick wins provide an organization the impetus for additional progress.
Implementing change and then sustaining it involves efforts to prevent regression. A strong change management plan must consider the practical steps of engagement and communication - success factors that are often overlooked.
Practicalities of Change
Leadership matters. Changing an organizational culture is challenging. Change management requires the creation of a vision, a strategic plan and tactical expectations. Employee “buy-in” driven by consistent, concise and frequent communications is necessary. A leader may be required to remove deviating personnel from their positions.
Inclusion matters. Make sure that physicians and end users who will be affected by the change are involved at the beginning before plans are drawn up and any decisions are made. Consider how to enable participation at all stages of change, including planning, decision-making and implementation. Communicate your thoughts and ideas clearly, avoiding jargon, and present any materials in a reader-friendly and accessible format.
Time matters. Understanding the physician’s schedule and competing priorities is essential. Make sure that practical arrangements enable involvement and avoid interruptions to the physicians’ clinical responsibilities. Simple logistical planning should consider accessible venues and alternative formats such as video conferences. Time of day, and day of week, should suit the stakeholder’s schedule. In some cases, consider financial implications when attendance at meetings will have an impact on physician productivity.
By addressing the practical nature of inclusion and time, change can come about through regular and thorough consultation with affected stakeholders. Hold meetings regularly so that people are more confident when giving their views. You can break down barriers and boundaries and open a two-way relationship by recognizing that everyone has an essential role in the process.
Footnotes:
1: 2018 Survey of America’s Physicians: Practice Patterns and Perspectives. The Physicians Foundation. https://physiciansfoundation.org/wp-content/uploads/2018/09/physicians-survey-results-final-2018.pdf
2: Ibid; Q17, page 15
3: Ibid; Q36, page 19
4: Ibid; Q15, page 14
5: Ibid; Q26, page 17
6: Ibid; Q13, page 14
7: JO Prochaska, WF Velicer. The Transtheoretical Model of Health Behavior Change Am J Health Promotion; Sept-Oct 1997. https://pubmed.ncbi.nlm.nih.gov/10170434/
8: Behavioral Change Models: Theory of Planned Behavior. https://sphweb.bumc.bu.edu/otlt/mph-modules/sb/behavioralchangetheories/BehavioralChangeTheories3.html
9: Bandura, A. (1989). Social cognitive theory. In R. Vasta (Ed.), Annals of child development. Vol. 6. Six theories of child development (pp. 1-60). Greenwich, CT: JAI Press. https://www.uky.edu/~eushe2/Bandura/Bandura1989ACD.pdf
10: Social network theory. University of Colorado. https://is.theorizeit.org/wiki/Social_network_theory
11: P. Lally, C. Jaarsfeld, H. Potts, J. Wardle. How Are Habits Formed: Modelling Habit Formation in the Real World. European Journal of Social Psychology; July 16, 2009. http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.695.830&rep=rep1&type=pdf
12: ADKAR Model of Change. https://www.toolshero.com/change-management/adkar-model/
13: Enduring Ideas: The 7-S Framework. McKinsey Quarterly; March 1, 2008. https://www.mckinsey.com/business-functions/strategy-and-corporate-finance/our-insights/enduring-ideas-the-7-s-framework
14: Bridges Transition Model. William Bridges Associates. https://wmbridges.com/about/what-is-transition/
15: Matt Donovan. The Eight Stages of Successful Large-Scale Change adapted from “The Heart of Change” by John Kotter; August 21, 2008. https://hbr.org/2008/08/the-eight-stages-of-successful.html
Related Insights
Related Information
Published
January 28, 2022
 Key Contacts
Key Contacts
Managing Director


