Modernizing the Funds Flow Process at Academic Medical Centers
Shifting a transactional process into a collaborative, strategic planning process
-
December 13, 2022
-
Known for being one of the most contentious topics between Academic Medical Centers (“AMC”s) and faculty practice plans (“FPP”s), the Funds Flow process is often seen as untouchable at most medical systems.1 Typically rife with legacy agreements, handshake deals with little to no documentation, and a patchwork of agreements tacked on from one Department Clinical Chief to the next, Funds Flow can be a political minefield at an academic medical system. However, as Sun Tzu wisely said: “In the midst of chaos, there is also opportunity.”2
In this article, the reader will find an overview of Funds Flow, the rationale and opportunities for modernization and proposed next steps.
Funds Flow Overview
Funds Flow is the process by which the AMC pays the faculty practice plan for strategically important and required operational services. Categories of Funds Flow can include:
- Medical directorships
- Administrative roles for providers
- Teaching and residency programs
- Research
- Providing hospital-based call coverage
Additionally, AMCs often subsidize the FPP’s net operating loss for new providers to ramp-up, for specific practices and/or specialties that the medical center views as imperative, and direct-employment hospital-based service lines (e.g., Anesthesiology).
Traditionally, the Funds Flow process is a behind-the-scenes task that the accounting team records as an intercompany journal entry booking the expenses to the AMC and the revenue to the FPP. However, approaching Funds Flow with this mindset ignores a key alternative whereby the AMC and FPP can use the process to collaborate and strategize on where to make key investments.
To make it a collaborative process, the AMCs must understand what they are paying for, how those amounts were calculated, and why they need the service they want the FPP to provide. On the flip side, the FPP should agree that the internal valuation of the services they are providing meets fair market standards and assures adequate compensation for all required and requested services.
Rationale for Modernization of the Funds Flow Process
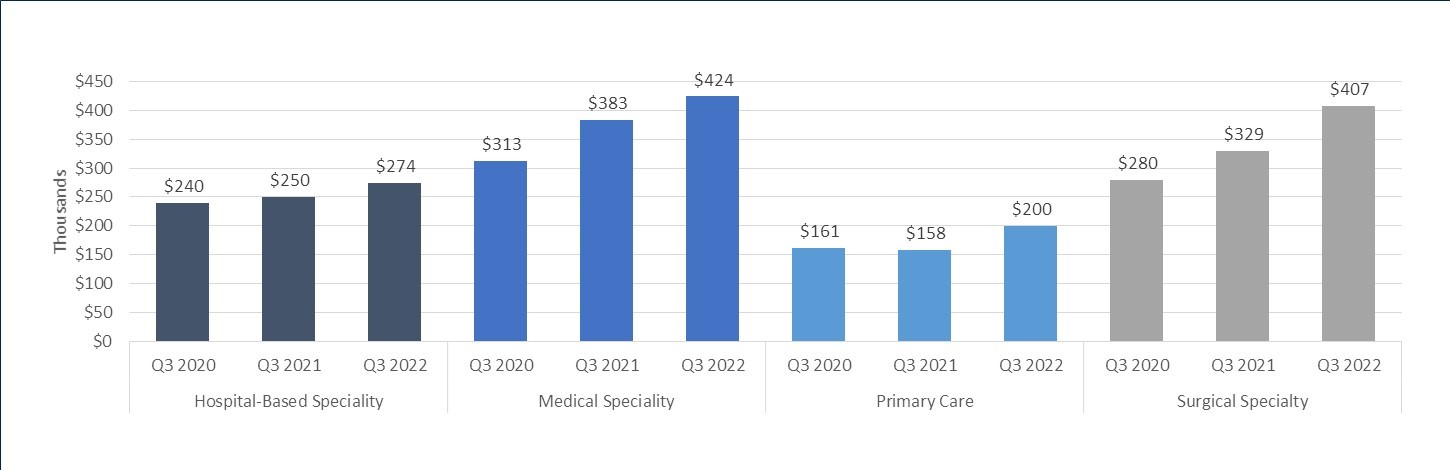
As health system margins get thinner and cash reserves shrink, now is a critical time to evaluate all areas of the organization, including how Funds Flow dollars are being spent. Mainly driven by physician compensation rising at a faster rate than reimbursement, the median subsidy (loss) per Physician FTE has climbed 21% year-over-year from $253,760 in 3Q21 to $306,404 in 3Q22.3,4,5 These climbing physician investment costs demand that the Funds Flow process, agreements, and methodologies be reevaluated and redesigned to ensure effective investments and furtherance of the system’s mission.
Median Subsidy (Loss) per Physician FTE by Specialty Cohort
Source: Kaufman-Hall, Physician Flash Report, October 2022, https://www.kaufmanhall.com/insights/research-report/physician-flash-report-october-2022
Modernizing the Funds Flow Process
If buy-in has been achieved at all the right levels to make changes to the functioning of the Funds Flow process, some key considerations require the attention of every AMC and FPP. If executed and managed well, implementing new tools, and streamlining processes can shift the Funds Flow process from a former back-end process into a mechanism for aligning the strategic planning efforts of the physician organization and the medical center. Here are some key items for consideration:
- Tracking and Administration
Funds Flow can be an unwieldy, cumbersome and time-consuming process for the finance team. It is imperative that the FPP have a well-designed database tool to house all Funds Flow agreements, which can be easily updated, reconciled, invoiced and ultimately recorded to the General Ledger. Microsoft Excel is well suited for this type of work; furthermore, the design of the spreadsheets can either add hours to the monthly close or be a catalyst in shortening the close calendar. - Approval and review processes
Depending on an organization’s preferred cadence, two different workstreams may be needed: (1) mid-year additions, changes and terminations; and (2) annual budgeting and planning process. In both instances, a formal in-take process should be incorporated along with a streamlined approval workflow. For the sake of transparency and accountability, team members from both the FPP and AMC should be included, and the resulting approvals should feed directly into the FPP finance team’s Funds Flow database downstream to record the journal entry and incorporate in the invoice. - Collaboration
A small, centralized group of key finance-team members from the FPP and AMC should understand: the process from beginning to end; the agreed-upon calculation methods for each category and arrangement; and the ability to educate others, including senior leadership, on the general guidelines behind the Funds Flow. Building transparency with room for open communication will generate trust between the groups and minimize points of contention. - Timeliness and accuracy
Agreed-upon deadlines for the monthly close, invoicing, and budget approval process must be maintained to give both finance teams enough time to coordinate and ensure accuracy. In view of the ongoing need for retroactive adjustments and quarterly/year-end reconciliations, finance teams should be sure to keep those adjustments clearly outlined in all agreed-upon Funds Flow guidelines.
Bottom Line
Given the increasing financial and operational pressures in a quickly evolving healthcare landscape, the time to turn over any stones is now. Yes, even that political boulder: Funds Flow. It is essential that organizations transition from the traditional, behind-the-scenes, transactional approach to Funds Flow and adopt a modernized Funds Flow model and approach capable of being leveraged to ensure maximally efficient and effective allocation of limited resources.
Reinventing the Funds Flow process does not need to be overly complicated. To do it well, organizations need:
- a mutually agreed-upon framework between the AMC and FPP;
- a dynamic, streamlined tracking tool to monitor and record Funds Flow more accurately; and
- a collaborative cross-company workgroup to keep the process operating smoothly.
Nevertheless, navigating the political minefield of Funds Flow can be a daunting task; but FTI Consulting is here to assist. Let the FTI Consulting team guide you on your journey to designing a more strategic and effective Funds Flow model for your organization.
Footnotes:
1: Satyan Lakshminrusimha, MD, FAAP, Susan Murin, MD, MSc, MBA. “Funds Flow Implementation at Academic Health Centers: Unique Challenges to Pediatric Departments.” The Journal of Pediatrics. (February 2, 2022). https://www.jpeds.com/article/S0022-3476(22)00089-0/fulltext
2: Sun Tzu. The Art of War. Translated by Lionel Giles. Published by Standard eBooks.
3: KaufmanHall. “The Current State of Hospital Finances: Fall 2022 Update.” American Hospital Association (September 15, 2022), https://www.aha.org/guidesreports/2022-09-15-current-state-hospital-finances-fall-2022-update.
4: Laura Dyrda. “Health System Cash Reserves Plummet.” Becker’s Hospital CFO Report (November 14, 2022), https://www.beckershospitalreview.com/finance/health-system-cash-reserves-plummet.html.
5: Kaufman-Hall. “Physician Flash Report October 2022.” (November 3, 2022) https://www.kaufmanhall.com/insights/research-report/physician-flash-report-october-2022
© Copyright 2022. The views expressed herein are those of the author(s) and not necessarily the views of FTI Consulting, Inc., its management, its subsidiaries, its affiliates, or its other professionals.
Published
December 13, 2022
 Key Contacts
Key Contacts
Managing Director